Ambriel vs Assured
Side-by-side comparison to help you choose the right tool.
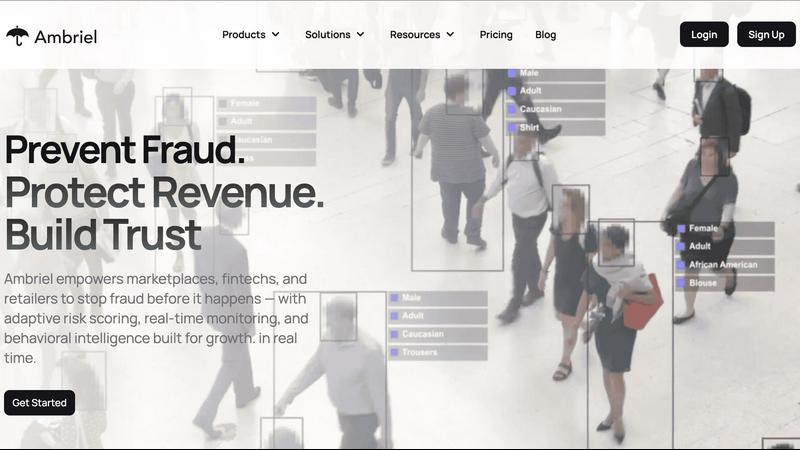
Ambriel stops fraud in real time to protect your revenue and build customer trust.
Last updated: March 1, 2026
Assured
Assured uses AI to automate provider credentialing and enrollment so healthcare companies can start billing in days, not months.
Visual Comparison
Ambriel
Assured
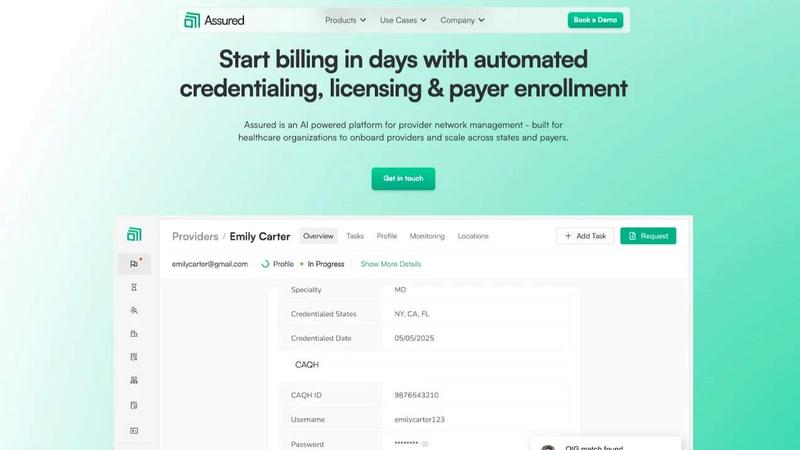
Overview
About Ambriel
In today's digital economy, businesses face a relentless and sophisticated threat: fraud. The challenge is twofold. You must protect your revenue and customer trust from bad actors, but doing so cannot come at the cost of a clunky, frustrating experience for your legitimate users. Manual reviews are slow and unscalable, while rigid rule-based systems create friction and false positives. This is where Ambriel provides the essential solution. Ambriel is a cutting-edge fraud intelligence and risk management platform designed to empower digital businesses to operate securely while adhering to regulatory requirements. It serves as a comprehensive shield for industries like fintech, marketplaces, retail, iGaming, and crypto, where transaction velocity and user trust are paramount. The platform's core value proposition is its powerful, unified ecosystem that combines advanced behavioral analytics, device intelligence, sanctions screening, and real-time AI-driven risk scoring. This allows organizations to proactively detect, score, and prevent fraud—from payment fraud and synthetic identities to bonus abuse and money laundering—before it impacts revenue or reputation. By analyzing a holistic view of transactions, user behaviors, devices, and network signals, Ambriel uncovers hidden risk patterns and automates mitigation, enabling businesses to prevent fraud, protect revenue, and build trust seamlessly.
About Assured
Assured is an AI-powered provider network management platform built to help healthcare organizations scale efficiently and stop losing revenue to administrative delays. It automates the complex, manual processes of credentialing, licensing, payer enrollment, and ongoing network monitoring. Designed for provider groups, health systems, payers, and digital health companies, Assured tackles the core problem of disconnected data and slow, error-prone manual work. Its core value proposition is dramatic speed and accuracy: get providers credentialed in 48 hours instead of 60+ days, achieve 95% first-pass approval rates for payer enrollments, and detect sanctions 22 days earlier than manual methods. As an NCQA-certified Credentials Verification Organization (CVO), Assured leverages AI to verify credentials across 2,000+ primary sources in parallel, auto-generate applications, and submit directly to payer portals. This means faster provider onboarding, quicker revenue generation, and complete peace of mind with real-time data monitoring, all from a single, centralized platform.